- Blog
- Battle tank ascii text art
- Free google sheets expense template monthly
- Stick ranger cavern 2
- Avigilon control center player free
- Battleship game online free against computer
- Sanctuary rpg black edition save editor
- Dragon age inquisition glyphs ancient baths
- Density of water in g
- 2048 x 1152 cool youtube banners
- Florida time zone map
- Ps3 eye camera driver windows 10
- Is decibels a logarithmic scale
- Bohemian rhapsody sheet music piano easy pdf
- Who developed the atomic theory
- What window command copies text
- Cavalier king charles spaniel seattle rescue
- Stanley sharpshooter staple gun not working
- Transparent background crosshairs png
- Space shuttle endeavour simulator ride
- Online color picker from image
- Best automatic pool covers
- Remington model 12 serial number dates
- Red hair highlighting coloring ideas
- Medicare abcd cost
- Google chrome webstore themes
- Space shuttle endeavour vertical display
- Play bejeweled 2 deluxe free
- Play game 2048 online
- Pc anime dancing live wallpaper free download
- Implementation of AGV robots
- Ivory ella elephant ivory ella elephant outline
- Mp3 to midi free converter download
- Free coins for solitaire tripeaks
- Gta v zombie apocalypse mod
- World of warships tanz skins
- Free licensed practical nurse resume template downloads
- Tattoo font letter examples
- Adage script font free
- Professional word document resume template
- Wedding ring box
- Frcp motion to dismiss
- Propresenter background loops free
- Queen victoria hemophilia family tree
- Rfactor 2 dx12 night tracks
- Hot incent sex stories in urdu
- Transfer media files from android to windows
- Free printable coordinate graphing pictures worksheets
For that reason, Medicare Advantage PPO plans list one out-of-pocket maximum amount for in-network services, and one out-of-pocket maximum amount that combines in-network and out-of-network healthcare costs. Both types have provider networks, but PPO plans typically pay a percentage of your healthcare costs when you see an out-of-network provider. There are several different types of Part C plans, including HMOs (Health Maintenance Organizations) and PPOs (Preferred Provider Organizations). The Medicare out-of-pocket maximum for Part C plans is established by the insurer that manages the plan. Part C plans are sold by Medicare-approved private insurers for this purpose. Many Part C plans also offer lower out-of-pocket limits of $6,000 or less. For in-network services in 2021, the highest Medicare out-of-pocket maximum a Part C plan could allow was $7,550.
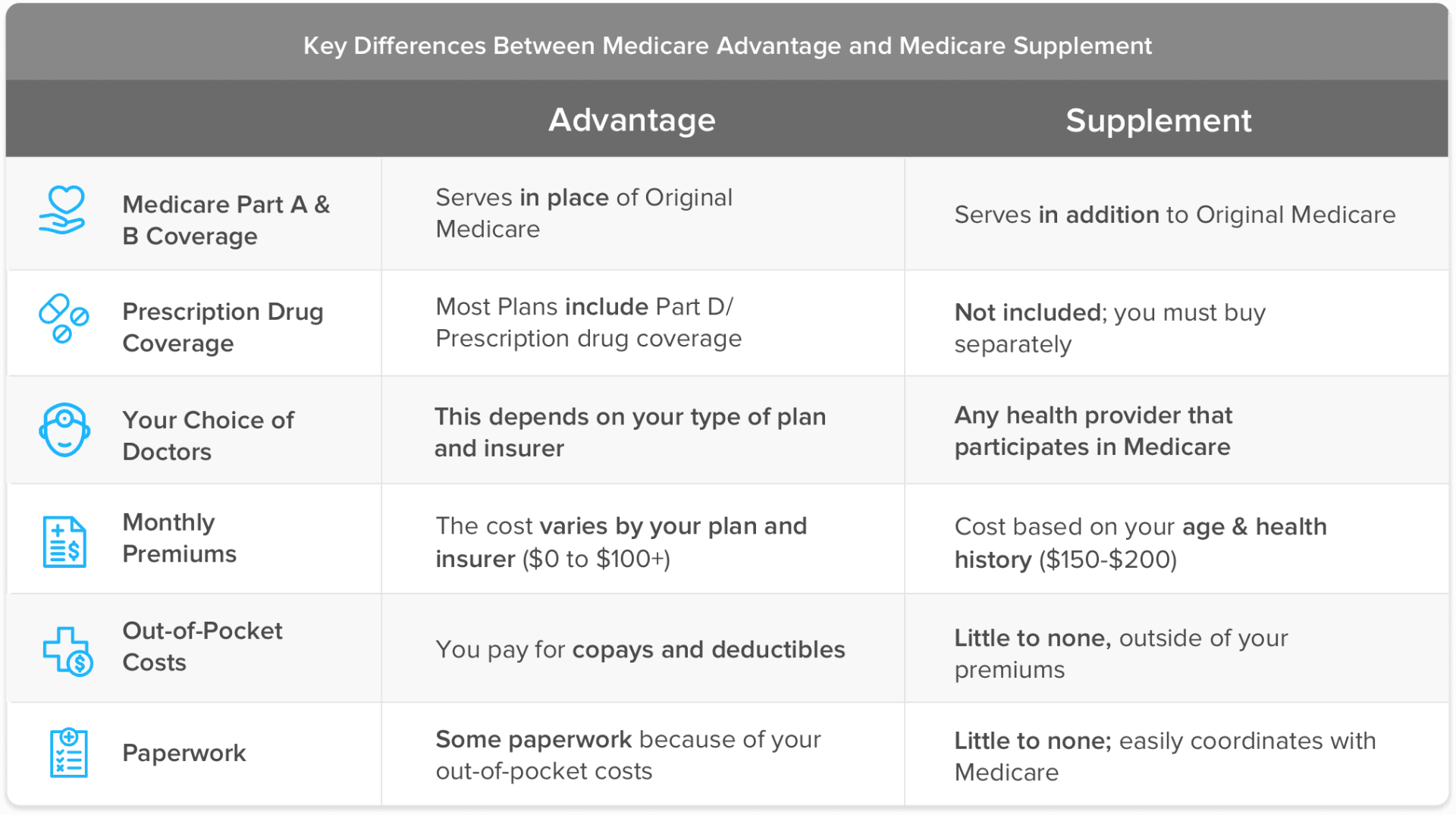
This means there is an automatic limit on the amount of money you will spend for covered healthcare during any given year. Unlike Original Medicare, Part C plans are required to have out-of-pocket maximums. Medicare Advantage plans are an alternative way to get full Medicare coverage.
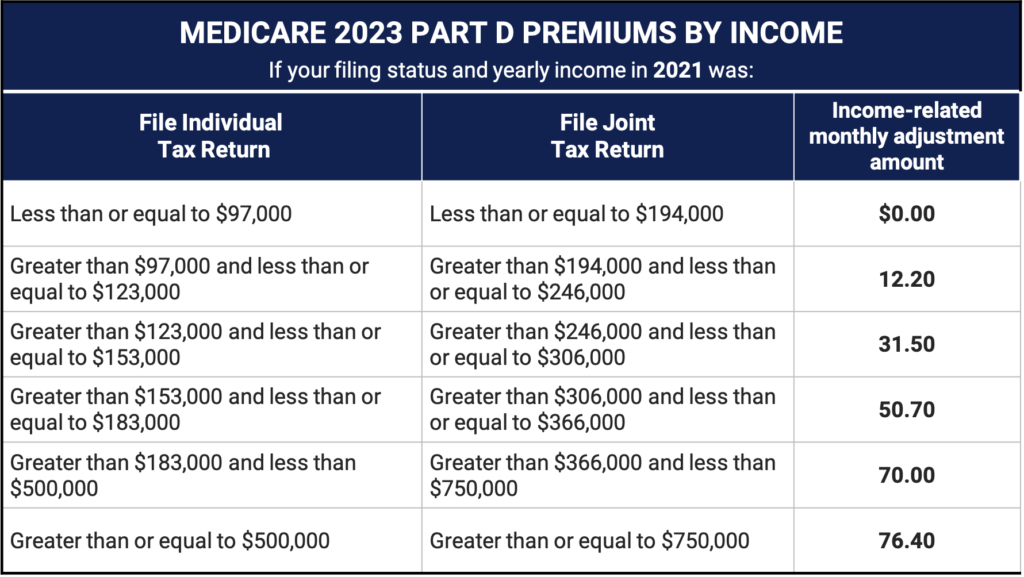
Instead of Original Medicare you may have, or be interested in getting, a Medicare Advantage (Part C) plan. If you have Original Medicare, there’s no ceiling on the amount of money you may have to pay for covered inpatient or outpatient services. Original Medicare consists of two parts - Part A and Part B. Many people are surprised to learn that Original Medicare doesn’t have out-of-pocket maximums.
- Blog
- Battle tank ascii text art
- Free google sheets expense template monthly
- Stick ranger cavern 2
- Avigilon control center player free
- Battleship game online free against computer
- Sanctuary rpg black edition save editor
- Dragon age inquisition glyphs ancient baths
- Density of water in g
- 2048 x 1152 cool youtube banners
- Florida time zone map
- Ps3 eye camera driver windows 10
- Is decibels a logarithmic scale
- Bohemian rhapsody sheet music piano easy pdf
- Who developed the atomic theory
- What window command copies text
- Cavalier king charles spaniel seattle rescue
- Stanley sharpshooter staple gun not working
- Transparent background crosshairs png
- Space shuttle endeavour simulator ride
- Online color picker from image
- Best automatic pool covers
- Remington model 12 serial number dates
- Red hair highlighting coloring ideas
- Medicare abcd cost
- Google chrome webstore themes
- Space shuttle endeavour vertical display
- Play bejeweled 2 deluxe free
- Play game 2048 online
- Pc anime dancing live wallpaper free download
- Implementation of AGV robots
- Ivory ella elephant ivory ella elephant outline
- Mp3 to midi free converter download
- Free coins for solitaire tripeaks
- Gta v zombie apocalypse mod
- World of warships tanz skins
- Free licensed practical nurse resume template downloads
- Tattoo font letter examples
- Adage script font free
- Professional word document resume template
- Wedding ring box
- Frcp motion to dismiss
- Propresenter background loops free
- Queen victoria hemophilia family tree
- Rfactor 2 dx12 night tracks
- Hot incent sex stories in urdu
- Transfer media files from android to windows
- Free printable coordinate graphing pictures worksheets
